You’ve probably never discussed this at dinner parties. Actually, you’ve probably never discussed this with anyone—not your doctor, not your partner, definitely not your mother.
But here you are, Googling “why do I have to lean back to poop” like it’s a normal Tuesday, and honestly? It’s more common than you’d think.
If you’ve discovered that reclining on the toilet is the only way you can actually pass stool without feeling like you’re trying to squeeze a watermelon through a garden hose, you’re not imagining things. Your body is telling you something. And no, that something isn’t “you’re weird.”
Let’s talk about what’s actually going on down there, why your body might prefer this unconventional position, and when it’s time to loop in a professional.
Quick Answer: Why You Feel Better Leaning Back
Here’s the short version: leaning back often compensates for pelvic floor or posture issues. It’s not the “wrong way” to poop—it’s your body’s workaround for something that isn’t functioning optimally.
Many people lean back because their pelvic floor muscles don’t relax properly in a standard sitting position. Instead of releasing to let stool through, these muscles stay tense or even tighten more when you try to push.
What leaning back does:
- Slightly changes the anorectal angle (the bend between your rectum and anal canal)
- Shifts your pelvic tilting, which may reduce pressure on tender areas
- Alters how your abdomen and diaphragm work together to create downward pressure
- May help the anal sphincter relax in ways that forward-leaning doesn’t for your particular body
But here’s the catch: Needing to lean back regularly may hint at underlying issues like pelvic floor dyssynergia, rectal descent, rectocele, or chronic constipation.
Occasional backward leaning? Usually fine. Daily difficulty, pain, or excessive straining that only improves when you recline? That warrants a closer look.
Key takeaway: Leaning back isn’t “wrong”—but if it’s the only way you can have a bowel movement without a struggle, something in your digestive system or pelvic area deserves attention.
How Pooping Is Supposed To Work (Anatomy 101)
Before we troubleshoot why you’re leaning backward, let’s cover what’s supposed to happen when everything works smoothly. Don’t worry—this won’t feel like a biology exam.
Your large intestine ends in the rectum, which is basically a storage area for stool before it exits. Below the rectum is the anal canal, which leads to the anus (the anal opening). When it’s go-time, your rectum contracts and pushes stool downward while your sphincter muscles and pelvic floor relax to let it through.
Here’s where it gets interesting: there’s a muscle called the puborectalis that wraps around your rectum like a sling. At rest, this muscle pulls the rectum forward and creates a kink—the anorectal angle. Think of it like a bent garden hose. When the hose is kinked, water can’t flow freely. Sitting on a modern Western toilet doesn’t allow the kink in your bowel to fully straighten, meaning that you may need to strain more to get a bowel movement out.
When you sit down to poop:
- The rectum fills and sends signals to your brain saying, “Hey, it’s time”
- Ideally, the puborectalis relaxes, which straightens the anorectal angle
- Your pelvic floor muscles lengthen and release
- Your anal sphincter opens
- Stool passes without you turning purple from straining
- Squatting straightens the anorectal angle, relaxing the rectal muscles and uses gravity to assist in elimination.
Posture matters because it directly affects how easily that angle can straighten. Research suggests the best position for bowel movements is one that straightens the anorectal angle, such as squatting or using a footstool. Leaning forward (or squatting) tends to help most people. Leaning backward? That’s where things get more complicated.
Picture it like this: imagine a side view of your body sitting on a toilet. The rectum angles forward toward your belly. Relaxing the puborectalis and leaning forward straightens that bend, creating a more direct exit path.
Why Leaning Back Feels Like It Helps
So if leaning forward is supposed to be better, why does leaning back feel like the magic solution for you?
Leaning backward shifts your pelvic position and changes how pressure distributes through your abdomen. For some bodies, this subjectively feels relieving—even if it’s not what the textbooks recommend.
What happens when you lean back:
Physical Change | Potential Effect |
|---|---|
Pelvis tilts backward | Alters the pull on the puborectalis muscle |
Spine extends | Changes how you generate intra-abdominal pressure |
Weight shifts | May reduce pressure on hemorrhoids, anal fissures, or a tender perineum |
Glutes and lower back relax | If these areas are chronically tight, releasing them may indirectly help pelvic floor muscles relax too |
Some people with chronic glute or low-back tightness naturally slump or recline, which changes abdominal pressure patterns in ways that accidentally help stool move.
Forward vs. backward lean—the typical experience:
- Most people find that leaning forward with knees higher than hips makes them feel like things “open up” more easily; forward-leaning with elevated knees (like a squat) is generally more effective for straightening the colon.
- Some people (like you, perhaps) find forward leaning creates more tension, discomfort, or a sense of being “blocked”
- Leaning back may provide temporary relief, but relying on it daily can signal that muscles and mechanics aren’t working efficiently
A straightened pathway leads to easier, more complete emptying with less straining, which can reduce the risk of issues like hemorrhoids or fissures.
It’s not inherently dangerous. But it might be a clue worth investigating.
Adopting the right posture can lead to improved bowel health and easier elimination by allowing your body to work with its natural mechanics.
Common Reasons You Have To Lean Back To Poop
Multiple overlapping factors can make backward-leaning feel like the “only” way that works. Let’s break down the usual suspects.
Pelvic Floor Dyssynergia (Anismus)
This is when your pelvic floor muscles and anal sphincter muscles do the opposite of what they should. Instead of relaxing when you push, they tighten—essentially closing the door you’re trying to open.
Leaning back may be an unconscious workaround that helps these muscles release. It’s like your body discovered a backdoor solution (pun intended).
Rectal Descent and Rectocele
Rectal descent means the rectum has dropped lower than it should. A rectocele (more common in women, especially after childbirth) is when the rectal wall bulges into the vaginal wall.
Both conditions can create a “pocket” where stool gets trapped. Leaning back might shift this blockage momentarily, allowing you to pass stool that otherwise feels stuck.
Chronic Constipation
When stool is hard, dry, and slow-moving—often from low fiber intake, dehydration, or certain medication—you need different mechanics to find leverage. Soft stool slides out easily in almost any position. Hard stool? That’s a negotiation.
Common symptoms of constipation that push people toward posture experiments:
- Straining for more than a few minutes
- Feeling like you can’t completely empty your bowels
- Having fewer than three bowel movements per week
- Stool that’s lumpy, hard, or painful to pass
Pregnancy and Postpartum Changes
Someone who had a baby in 2020 and has struggled with bathroom visits ever since isn’t imagining things. Pregnancy stretches pelvic supports, and vaginal delivery can further affect the pelvic floor, rectum, and even the position of the uterus.
The ideal poop position may literally be different after childbirth. Many women find their previous bathroom routine no longer works.
Spine and Hip Issues
Low-back pain, hip stiffness, prior surgery, or conditions like sciatica can make the “textbook” forward lean genuinely uncomfortable. If leaning forward causes pain, your body naturally avoids it—leaving backward leaning as the only tolerable option.
Leaning Back vs Leaning Forward: What Research And Therapists Recommend
Here’s what the evidence actually says: most pelvic floor therapists and clinical studies favor a forward-leaning, knees-up posture for efficient, low-strain defecation.
The ideal poop position according to research:
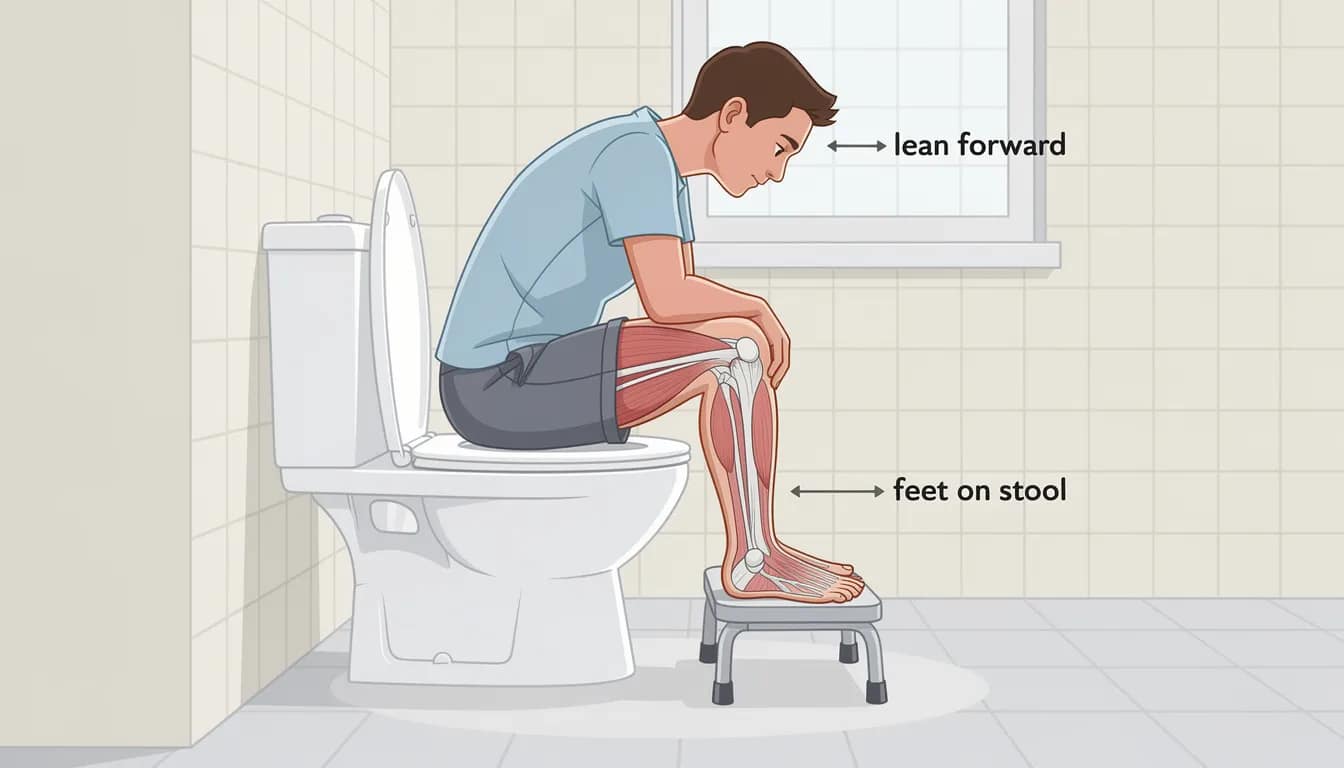
- Feet flat and elevated on a foot stool (or a Squatty Potty, stack of books, yoga blocks—whatever you’ve got)
- Knees higher than hips
- Torso leaning slightly forward, with elbows resting on knees
- Spine relatively neutral, not slumped
- Pelvic floor relaxed, not clenched
Using a footstool that lifts the knees higher than the hips recreates the squatting posture and straightens out kinks in the rectum.
This position simulates squatting, which humans did for thousands of years before modern toilets came along. Studies dating back to the 1980s comparing squatting versus sitting toilets consistently show faster, less-strained bowel movements in squat-like positions.
A 2019 study found that using a toilet posture modifier (like a foot stool) reduced bowel movement duration and straining while increasing the sense of complete evacuation. Incorporating a footstool to achieve the squatting posture can eliminate the need to lean back for many people.
What therapists observe:
Pelvic floor physical therapists frequently note that patients who must lean back or rock to have a bowel movement often have underlying coordination problems. The backward lean might be helping despite suboptimal mechanics, not because of optimal ones.
The nuanced take: Leaning back isn’t “wrong.” But if it’s the only way you can poop without straining, it’s worth investigating why—because there may be a solution that works even better.
How To Find A Better Poop Posture (Step-By-Step)
Experimenting with posture is safe for most people, and small changes can make a surprisingly big difference. Here’s how to find what works for your body.
The Supported Squat Position (Step-by-Step)
- Elevate your feet. Place them on a 6–9 inch stool, a stack of books, or a dedicated product like a Squatty Potty. You want your knees higher than your hips.
- Lean slightly forward. Rest your elbows on your knees or thighs. This doesn’t have to be dramatic—even a 15-20 degree forward tilt helps.
- Relax your belly. Stop sucking in your abdomen. Let it go soft. Seriously—nobody’s judging your stomach right now.
- Breathe into your belly. Take slow, deep breaths using your diaphragm (belly breathing, not chest breathing). This helps signal your pelvic floor and anal sphincter to relax and open.
- Don’t push hard. Instead of bearing down like you’re trying to lift a car, think about gently widening your pelvic floor. Some therapists suggest imagining you’re “blowing up a balloon” in your lower belly.
- Keep it short. Limit your toilet time to 5–10 minutes. Prolonged sitting (hello, phone scrolling) creates pressure on the pelvic area and can worsen hemorrhoids.
Fine-Tuning Your Position
Try forward-leaning first with elevated feet. If that still feels blocked, experiment with:
- Very mild backward rocking (not a full recline)
- Slight side-to-side shifting
- Different heights for your foot stool
Pay attention to which posture reduces straining the most. Your body will give you feedback.
When Leaning Back Is A Red Flag: Symptoms To Watch For
Posture alone usually isn’t dangerous. But certain symptoms combined with reliance on unusual positions to control bowel movements need medical attention.
Alarm Signs That Warrant Urgent Evaluation
- Rectal bleeding not linked to known hemorrhoids
- Unexplained weight loss
- Anemia (fatigue, paleness, shortness of breath)
- Severe new-onset constipation after age 50
- Sudden severe abdominal pain
- Vomiting with inability to pass gas or stool (possible blockage—seek emergency care)
Symptoms Suggesting Rectal Descent or Rectocele
- Feeling a bulge inside the pelvis
- Needing to press on the vagina or perineum to pass stool
- A sense that the rectum is “dropping” or prolapsing
- Worsening symptoms with standing or at the end of the day
Signs of Pelvic Floor Dyssynergia
- Long toilet trips even when you feel the urge to go
- Needing to strain hard even for soft stool
- Frequent sensation of incomplete emptying
- Feeling like you’re “pushing against a closed door”
Other Symptoms That Need Professional Review
- Persistent pain during or after bowel movements
- Fecal incontinence (leakage)
- Mucous drainage from the anus
- Discomfort that interferes with daily activities
Don’t ignore these. Your body is communicating something that goes beyond posture.
How Doctors Diagnose Pelvic Floor and Rectal Problems
If your symptoms suggest something more than simple constipation, your doctor will work to rule out structural disease and evaluate how well your muscles coordinate during defecation.
Common Diagnostic Steps
Test | What It Involves | What It Checks |
|---|---|---|
Digital rectal exam (DRE) | Doctor inserts a gloved, lubricated finger into the rectum | Muscle tone, coordination, masses, tenderness |
Sigmoidoscopy or colonoscopy | Camera on flexible tube examines the colon and rectum | Structural issues, polyps, inflammation, tumors |
Anorectal manometry | Small catheter measures pressure in the anal canal | How well sphincter muscles relax and contract |
Balloon expulsion test | Small balloon inserted in rectum; you try to push it out | Whether you can effectively evacuate |
Defecography | X-ray or MRI while passing contrast material | Visualizes anorectal angle, rectal prolapse, rectocele |
Important: Most diagnoses are based on at least two converging test results plus your symptoms—not just one abnormal finding.
These tests might sound embarrassing, but they’re routine, brief, and crucial for getting the right treatment. Medical professionals have seen it all. Your comfort and proper diagnosis matter more than momentary awkwardness.
Treatment Options If You Always Need To Lean Back
Treatments are individualized based on what’s causing your symptoms. To effectively treat constipation, approaches may include lifestyle changes, medications, and seeking medical advice. Work with a healthcare professional to create the right plan for you.
Pelvic Floor Physical Therapy
Specialized pelvic floor therapists teach you how to relax, coordinate, and correctly use your rectal muscles and pelvic floor during defecation. This isn’t your typical gym workout—it’s retraining your body to do what it should do automatically.
Many patients see significant improvement. Someone who spent years straining and leaning back might learn, within weeks of therapy, that a simple breathing technique and posture adjustment changes everything.
Biofeedback Therapy
Sensors placed near the pelvic floor muscles provide real-time feedback on a screen. You can actually see when you’re tensing versus relaxing, which helps retrain the nerves and muscles involved in defecation.
This is particularly effective for pelvic floor dyssynergia.
Lifestyle Changes
- Hydration: Drink enough water throughout the day (aim for pale yellow urine)
- Fiber: Work up to 20–30 grams daily, adapted to your tolerance
- Regular exercise: Movement stimulates the colon and promotes healthy bowel habits
- Consistent toilet routine: Go when you feel the urge; don’t chronically delay
Medication Strategies
- Stool softeners help make stool easier to pass
- Osmotic laxatives draw water into the colon
- Prescription options exist for more stubborn cases
Always use these under guidance—long-term unsupervised laxative use can create other factors that worsen bowel function.
Surgical Options
For conditions like severe rectal prolapse, significant rectocele, or rectal descent that don’t respond to conservative treatment, surgery may be recommended. This is typically a last resort when other measures haven’t provided relief.
Practical At-Home Tips To Make Pooping Easier Today
While you’re figuring out the bigger picture, here are non-invasive strategies to try right now.
Quick Wins for Better Bathroom Visits
- Use a footstool. Even if you still prefer a slight lean back, elevating your feet changes the game. A stable foot stool, stack of books, or low box works.
- Time it right. Try sitting on the toilet after breakfast or a warm drink. The gastrocolic reflex naturally increases colon activity after eating.
- Try abdominal self-massage. Gently massage your abdomen following the colon’s path: up the right side, across the top, down the left side. This can stimulate movement through your large intestine.
- Skip the chronic straining. Breath-holding and pushing hard for extended periods aggravate hemorrhoids and strain the pelvic floor. If nothing’s happening after 5–10 minutes, get up and try again later.
- Put down the phone. Prolonged toilet sitting creates unnecessary pressure on the pelvic area. Set a timer if needed.
- Stay hydrated. Drink more water throughout the day—especially if you’re increasing fiber intake.
- Move your body. Regular exercise, even walking, helps keep your bowels moving.
Listen to Your Body
These tips can help, but they’re not substitutes for medical evaluation if symptoms persist or worsen. If you’ve tried lifestyle changes, adjusted your posture, and still find yourself depending on unusual positions or excessive straining, it’s time to involve a professional.

When To Talk To A Professional (And What To Ask)
Recurring trouble with bowel movements or dependence on unusual postures is a valid reason to seek help. You’re not overreacting. You’re not being dramatic. This is literally what doctors are for.
Where to Start
- Primary care physician: Can evaluate symptoms, rule out obvious issues, and refer you
- Gastroenterologist: Specializes in the digestive system and can order advanced testing
- Colorectal surgeon: Evaluates structural problems like rectal prolapse
- Pelvic floor physical therapist: Addresses muscle coordination and retraining
Questions to Ask
- “Could I have pelvic floor dyssynergia?”
- “Should I be evaluated for rectal descent or rectocele?”
- “Would pelvic floor physical therapy help my situation?”
- “Are there other factors contributing to my symptoms?”
How to Prepare for Your Appointment
Track your symptoms for 1–2 weeks before your visit:
- How often do you need to lean back or rock?
- Rate your straining level (1–10)
- Note your stool consistency (use the Bristol Stool Chart)
- Record how long you typically sit on the toilet
- List any pain, bleeding, or other symptoms
Mention relevant history:
- Childbirth (especially difficult vaginal deliveries)
- Pelvic surgeries
- Neurological conditions
- New or chronic medication that might affect bowel function
- History of constipation or fecal incontinence
The Encouraging News
It’s possible to retrain bowel habits and improve comfort. Pelvic floor dysfunction, chronic constipation, and even some structural issues respond well to treatment when properly diagnosed. You don’t have to “just live with it.”
Your body isn’t broken—it’s asking for a different approach. And once you find what works, those bathroom visits become a whole lot less of an ordeal.
Ready to stop fighting your body on the toilet? Start with a foot stool, try the supported squat position, and if things don’t improve within a few weeks, make that appointment. Your future self—the one who poops efficiently and gets on with their day—will thank you.

